The current medical treatment options for androgenetic alopecia
(AGA), although effective, tend to show a plateauing-off of the
response with no further hair growth.1 Hair transplantation is
unacceptable to many patients owing to it being a surgical
modality and/or the cost involved.
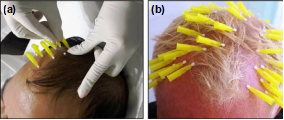
Polydioxanone (PDO) threads have emerged popular for
non-surgical face lift. Foreign body reaction-induced neocollagenesis, mechano-transduction (mechanical stimuli-induced
fibroblastic response), regulation of gene expression and
improved microcirculation seem to be the plausible mechanisms.2
Microneedling using a dermaroller is another efficacious facial
rejuvenation procedure that creates cutaneous micropunctures
with release of growth factors such as platelet-derived growth
factor (PDGF) and others.3,4 This effect has been extrapolated to
stimulate hair growth, confirmed by the results of a randomized
double-blind trial.4 Akin to this therapeutic strategy, we assessed
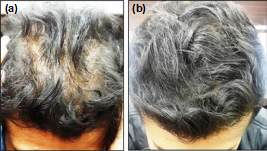
the response of male AGA to the scalp insertion of PDO threads.